
Countries cannot simply lock down their societies to defeat coronavirus, the World Health Organization’s top emergency expert said, adding that public health measures are equally needed to curb the proliferation of this virus.
Dr Mike Ryan said: “What we really need to focus on is finding those who are sick, those who have the virus, and isolate them, find their contacts and isolate them,” in an interview on the BBC’s Andrew Marr Show.
In the year 2012, On the World Malaria Day, WHO launched an initiative called T3: Test, Treat, Track, urging malaria-endemic countries, donors and the global malaria community to scale up diagnostic testing, treatment and surveillance for malaria. This framework was provided for the endemic countries to strengthen these three pillars of malaria control and elimination.
The recent inception of COVID-19 requires understanding transmission patterns. Cases and close contacts in the general population can be restricted to close settings (like households, health care settings, schools). For health workers in a health-care setting in which a confirmed case has received care. The WHO has envisioned that investigation will be conducted across several countries or sites with geographical and demographical diversity. It is the primary investigation protocol to be initiated upon identification of the initial laboratory-confirmed cases of COVID-19 in a country. Follow-up and testing of respiratory specimens and serum of health care workers within a facility in which a confirmed case of COVID-19 infection is receiving care can provide useful information on transmissibility and routes of transmission and are important for limiting amplification events in health care facilities.

“You can’t fight a virus if you don’t know where it is,”
WHO director general, Tedros Adhanom Ghebreyesus
“Find, isolate, test and treat every case, to break the chains of transmission.
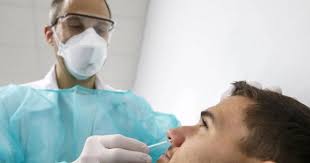
Large scale testing is needed to identify and isolate cases. It can also help provide evidence of how this virus affects people of different ages and genders. Prof Sunetra Gupta and a team of researchers at Oxford University, suggests that “only a very small proportion of the population is at risk of hospitalisable illness” and that more than half the population have already been exposed to the virus, largely without symptoms.
If this were true, we could expect a big surge of hospitalisations and deaths over the next six weeks, but then the epidemic would recede, probably with no second wave. But to know whether this is actually the case, we urgently need immunity tests that will show whether people have had the virus.
There is no vaccine to treat the Novel Corona virus yet. Researchers are currently working on creating a vaccine specifically for this virus. Antibiotics are also ineffective because COVID-19 is a viral infection and not bacterial.
If your symptoms are more severe, supportive treatments may be given by your doctor or at a hospital. This type of treatment may involve:
- fluids to reduce the risk of dehydration
- medication to reduce a fever
- supplemental oxygen in more severe cases
People who have a hard time breathing on their own due to COVID-19 may need a respirator.
Remdesivir is an experimental broad-spectrum antiviral drug originally designed to target Ebola. Researchers have found that remdesivir is highly effective at fighting the novel coronavirus in isolated cells.
Chloroquine is a drug that’s used to fight malaria and autoimmune diseases. Researchers have discovered that this drug is effective at fighting the SARS-CoV-2 virus in studies done in test tubes. Clinical trials are currently looking at the potential use of chloroquine as an option for combating the novel coronavirus.
With the surge in positive cases of the novel corona virus, the primary goal should be to curb the mass transmission along with tracing, testing and treating the infected.


Reblogged this on The Bleeding Ink.
LikeLike